At Dr. Tayyab saleem malik clinic (Cosmetic Enclave)
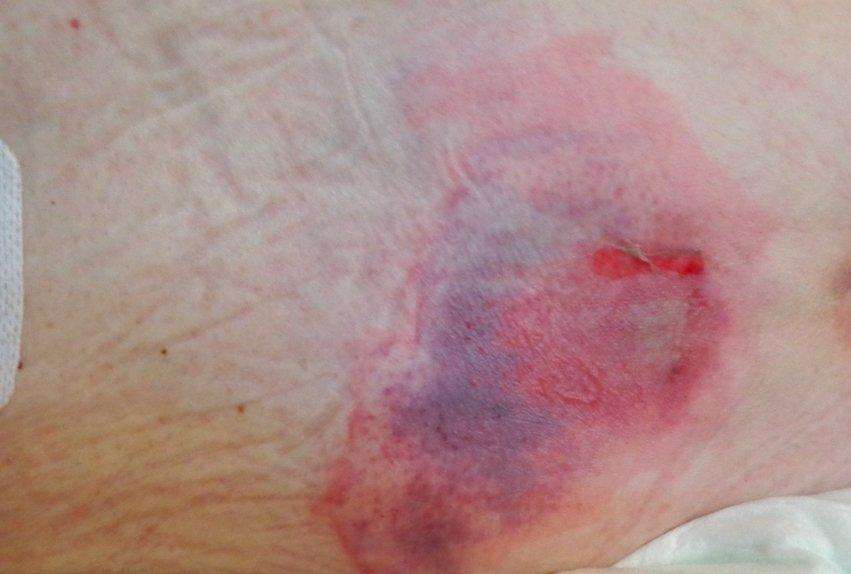
Pressure ulcers, also known as bed sores or pressure sores, are localized areas of damage to the skin and underlying tissues. They typically occur in individuals who have limited mobility and are unable to change their body positions frequently. Pressure ulcers develop when prolonged pressure, friction, or shearing forces are applied to certain areas of the body, primarily over bony prominences.
Common sites for pressure ulcers include the sacrum, heels, hips, and elbows, but they can develop anywhere on the body. The severity of a pressure ulcer is classified into different stages:
- Stage 1: The skin appears intact but shows non-blanchable redness, indicating potential damage to deeper tissues.
- Stage 2: The skin exhibits a partial-thickness loss, characterized by an open ulcer, shallow crater, or blister.
- Stage 3: The ulcer extends through the full thickness of the skin, exposing the underlying fat tissue. The wound may appear as a deep crater.
- Stage 4: The ulcer is deep, reaching the muscle, tendon, or bone. Extensive tissue damage is evident.
Pressure ulcers can cause significant pain, discomfort, and complications such as infection, cellulitis, or even sepsis. Prevention and early intervention are key in managing pressure ulcers effectively. Here are some preventive measures and treatment approaches:
- Frequent repositioning: Regularly changing the individual’s position, redistributing pressure, and relieving pressure on vulnerable areas.
- Adequate support surfaces: Using specialized pressure-relieving mattresses, cushions, or overlays to distribute pressure and reduce the risk of ulcer formation.
- Skin care: Maintaining good hygiene, keeping the skin clean and dry, and using appropriate moisturizers to prevent excessive dryness or breakdown.
- Nutrition and hydration: Ensuring a well-balanced diet with adequate intake of nutrients, especially protein, vitamins, and minerals, to support healthy skin and tissue healing.
- Education and awareness: Providing education to individuals and caregivers on the importance of skin care, proper positioning, and the early signs of pressure ulcer development.
- Wound management: For established pressure ulcers, treatment may involve regular wound cleaning, debridement of dead or infected tissue, application of appropriate dressings, and the use of advanced therapies if necessary.
- Infection control: Addressing and managing any infections associated with pressure ulcers through proper wound care, antibiotic therapy, or other interventions.
- Pain management: Providing pain relief measures, such as medications or topical treatments, to improve comfort and enhance the individual’s quality of life.
It is important to seek medical attention if a pressure ulcer develops, as healthcare professionals can assess the severity, identify any underlying issues, and provide appropriate treatment. Additionally, involving a multidisciplinary team consisting of wound care specialists, nurses, dieticians, and therapists can help optimize the management of pressure ulcers and promote healing.